
Location
-
The Primary Role of a Gastroenterologist
posted: Nov. 08, 2023.

-
Common Dietary Triggers of Digestive Issues: Identifying and Managing Your Triggers
posted: Mar. 23, 2023.

-
Colon Cancer Prevention: Identifying Warning Signs and Reducing Your Risk
posted: Mar. 14, 2023.
-
Common Gastrointestinal Disorders and Their Treatments
posted: Feb. 08, 2023.

-
The Benefits of Early Detection: How Colon Cancer Screening Can Save Lives
posted: Jan. 26, 2023.

-
Gastroesophageal Reflux Disease (GERD): Symptoms, Diagnosis, and Treatment
posted: Jan. 13, 2023.

-
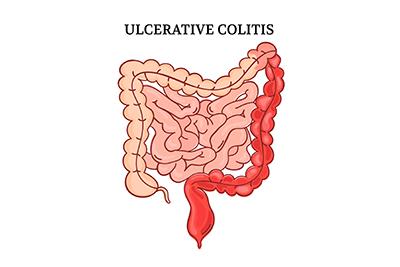
What Is Ulcerative Colitis?
posted: Dec. 28, 2022.
-
Understanding Liver Disease
posted: Dec. 09, 2022.

-
Are You Dealing With Loss of Appetite?
posted: Nov. 23, 2022.

-
Healthy Lifestyle With IBS
posted: Nov. 09, 2022.

-
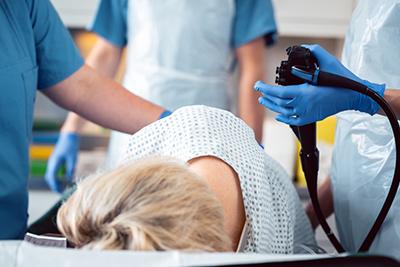
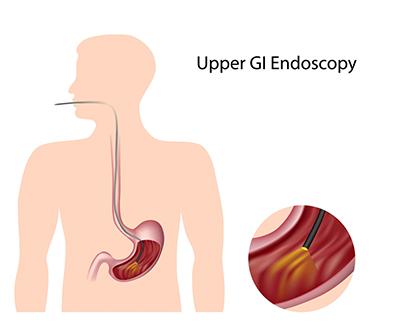
Reasons You May Need an Endoscopy
posted: Oct. 17, 2022.
-
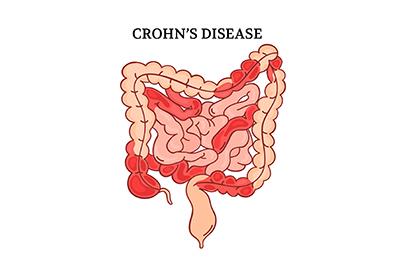
Are You Struggling With Crohn’s Disease?
posted: Oct. 01, 2022.
-
Why Is a Colonoscopy Recommended?
posted: Sep. 22, 2022.
-
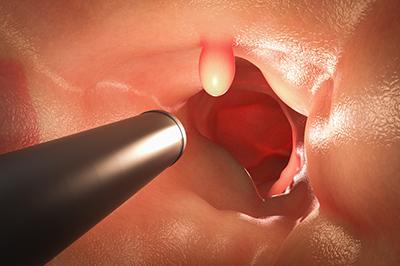
Benefits of Having a Gastroenterologist
posted: Sep. 08, 2022.
-
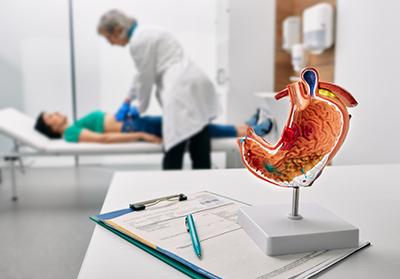
Common Causes of Heartburn
posted: Aug. 26, 2022.
-
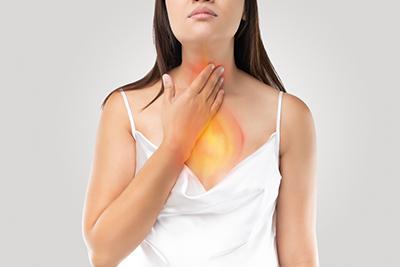
How Your Diet Affects Your Stomach Health
posted: Aug. 05, 2022.

